 Now, almost 25 million cases and over 400,000 deaths later, we stand by our comment at the time that such tweets were both irresponsible and dangerous. Eleven months later, we’re still paying the price for not taking things seriously.
Imagine if we had closed all borders at the time and asked everyone except essential workers to stay home for one month. Anyone who had been exposed at that point could have been quarantined and their contacts traced through a federally coordinated effort as was done in many other countries such as Australia, New Zealand, Singapore, etc.
Imagine having a chart shaped like either of these…
Now, almost 25 million cases and over 400,000 deaths later, we stand by our comment at the time that such tweets were both irresponsible and dangerous. Eleven months later, we’re still paying the price for not taking things seriously.
Imagine if we had closed all borders at the time and asked everyone except essential workers to stay home for one month. Anyone who had been exposed at that point could have been quarantined and their contacts traced through a federally coordinated effort as was done in many other countries such as Australia, New Zealand, Singapore, etc.
Imagine having a chart shaped like either of these…
 The cost for paying all those salaries for one month: about $400 billion. We could have reopened the country a month later with confidence. It has been estimated that we’ve spent over $16 trillion so far, and a full reopening is still months away at best.
Water under the bridge, of course. And maybe you’re one of the lucky ones who hasn’t yet been touched by COVID-19. Right now, one of every 34 Americans has an active case. One of every 13 people has been diagnosed. Former FDA Commissioner Scott Gottlieb said last month that about a third of Americans would ultimately be diagnosed. That was before the new, much more contagious strain was discovered.
Wouldn’t it be nice if we had taken it more seriously? Our current estimates call for over 450,000 deaths by the end of January and 500,000 by the end of February – at which point total cases should be around 30,000,000. Both might have already peaked; but, it will take a while for vaccines to get to market and for enough people to get vaccinated to make a difference.
Elsewhere in the world, things will unfortunately continue to get worse – especially for countries without the money and the healthcare infrastructure to stop the spread.
I’ll remove this “sticky” post from the front page for the time being. Coverage of the pandemic is very extensive now and there are many sources for great information. I’m praying there will be no need to return it to a place of any prominence.
UPDATE: October 20, 2020
The cost for paying all those salaries for one month: about $400 billion. We could have reopened the country a month later with confidence. It has been estimated that we’ve spent over $16 trillion so far, and a full reopening is still months away at best.
Water under the bridge, of course. And maybe you’re one of the lucky ones who hasn’t yet been touched by COVID-19. Right now, one of every 34 Americans has an active case. One of every 13 people has been diagnosed. Former FDA Commissioner Scott Gottlieb said last month that about a third of Americans would ultimately be diagnosed. That was before the new, much more contagious strain was discovered.
Wouldn’t it be nice if we had taken it more seriously? Our current estimates call for over 450,000 deaths by the end of January and 500,000 by the end of February – at which point total cases should be around 30,000,000. Both might have already peaked; but, it will take a while for vaccines to get to market and for enough people to get vaccinated to make a difference.
Elsewhere in the world, things will unfortunately continue to get worse – especially for countries without the money and the healthcare infrastructure to stop the spread.
I’ll remove this “sticky” post from the front page for the time being. Coverage of the pandemic is very extensive now and there are many sources for great information. I’m praying there will be no need to return it to a place of any prominence.
UPDATE: October 20, 2020
Herd Immunity: Doing the Math
In June, we observed that the US had embarked on a herd immunity approach to dealing with the COVID-19 pandemic.With little public discussion or debate, the US has embarked on a herd immunity approach to the coronavirus. No one’s really describing it as such, but the label is accurate just the same. Over the past month, scores of politicians and business leaders have declared (from the safety of their home offices) that “getting back to work” is more important than saving the maximum number of lives from COVID-19… Bottom line, the decision to reopen the country was made out of political and economic desperation with suspect motives and dubious scientific backing. While the strategy was purportedly for the benefit of the American worker, it is those very same workers who will end up paying the price.It was a provocative thing to say at the time, and I received a fair amount of blowback, most of it along the lines of “you’re exaggerating” or “not even Trump would do something like that.” At this point, it is patently obvious that the Trump administration has embraced herd immunity despite the enormous loss of life it would entail. Let’s do the math. Most advocates admit that herd immunity would require 60-70% of a country’s residents to become infected before protection would be afforded to the general population. In the United States, this would mean between 199-232M people becoming infected. We’ll go with the average of 215M. Compare this to the total known positive cases of about 8.5M and the likely 35M who have already been infected but not diagnosed, and the implication is that another 180M would have to be infected. The death rate has obviously fallen greatly over the past few months as those infected have tended to be younger and healthier and more effective therapeutics have been developed. But, it still hovers around 2.7% of diagnosed cases and 0.6% of probable cases. Applied to 180M infected, this would mean total deaths exceeding 1.1M. Unacceptable. The number of cases diagnosed each day is increasing at an increasing rate (i.e exponentially.) The 3-day moving average of new daily cases a month ago was 43,253. Today, it reached 58,133. A month from now it will reach 175,000 new cases and by the end of the year it will total well over 250,000 each and every day. The current 8.5M diagnosed will have grown to over 20M. Deaths now stand at 226,000. Daily deaths, which averaged less than 300 in June, are now topping 1,000 again and will reach 2,000 per day within the next month. By the end of the year, we will see over 310,000 total dead – more than were lost in The Gulf War, Spanish-American War, Iraq-Afghanistan, Mexican War, War of 1812, Revolutionary War, Korea, Vietnam and World War I put together. Sometime in February, total deaths will exceed the 405,000 lost in World War II. I know what you’re thinking. What about a vaccine? While it’s true that several companies are making excellent progress, it will be well into 2021 before any vaccine is widely available. It will be too late for the hundreds of thousands who will die needlessly between now and then. At 1 of every 10 Americans infected and 1 of every 740 Americans dead, it will be unusual not to know many who were sick and a few who died. It’s hard to talk about COVID-19 without talking about politics these days. Two days ago, new White House coronavirus advisor Dr. Scott Atlas tweeted that masks were not effective. It’s an opinion counter to that of the vast majority of scientists and doctors – including more than 100 of Atlas’ former colleagues at Stanford Medical School. President Trump’s rallies are testament to the disregard he has displayed for masks and social distancing. “It’s the last two weeks. Fuck it,” one Trump adviser said. People are indeed tired of the coronavirus – including masks, social distancing, remote learning, closed businesses, restaurants and stores, unemployment and staycationing. It’s getting old, it’s harming the economy, and it’s taking a toll on physical and mental health. But, for most of us, it beats dying. Even if you’re willing to take chances with your own life, it still beats killing grandma. In 1970 a Stanford psychologist studied the effect of delayed gratification by offering children a marshmallow. If they were able to abstain from eating it until he returned in 15 minutes, they were promised a second marshmallow. The study found that those who were able to delay gratification tended to have better life outcomes such as higher SAT scores and fewer behavioral problems. Though the study has been criticized over the years, its conclusion is worth taking to heart. It’s tempting to follow the advice of those “experts” and political “leaders” who insist we can ignore the risks and get back to normal life right now. It would be great. But, it would result in millions more sickened and hundreds of thousands dead. By taking modest precautions, exercising patience and delaying gratification, we can do better. Let’s not fail the marshmallow test. UPDATE: September 2, 2020 This is an excellent summary of where we are and why. More importantly, it offers simple, clear solutions to America’s coronavirus disaster. Reprinted from The New Yorker, September 2, 2020. We Can Solve the Coronavirus-Test Mess Now – If We Want To by: Atul Gawande
To get out of this pandemic, we need fast, easy coronavirus testing that’s accessible to everyone. From the way people often talk, you might think we need a technological breakthrough to achieve this. In fact, we don’t have a technological problem; we’ve got an implementation problem. We could have the testing capacity we need within weeks. The reason we don’t is not simply that our national leadership is unfit but also that our health-care system is dysfunctional.
Many developed countries have met their testing needs, and ready access to speedy tests has been key to containing outbreaks and resuming social and economic activity. Whether you live in England or South Korea, scheduling is straightforward. No doctor’s order is required. Tests, where indicated, are free. And you typically get results within forty-eight hours.The need for speed
The course of infection with the SARS-CoV-2 virus is relatively brief. It starts with perhaps as little as a few hundred viral particles getting into your respiratory passage; then, if they take hold, they multiply to a viral count so high that you are exhaling millions of viral particles per hour. You are typically at your most contagious around day five of infection. Symptoms usually begin about the same time. In more than eighty per cent of cases, adequate oxygen levels can be maintained without hospitalization, and the body’s immune system can reduce viral counts rapidly. In these mild to moderate cases, researchers have found almost no transmission a week after the onset of symptoms, although recovery takes upward of two to three weeks for a third of such patients. (In cases of serious illness, the reduction in viral counts can take a week or so longer.) The goal of testing is to detect the virus as early as possible during infection. The standard diagnostic test involves, as tens of millions of people now intimately know, a swab of the cavity deep behind the nasal passage—or, as more recently authorized by the Food and Drug Administration, of just inside the nose. A few labs have been approved to test saliva. The sample from the patient is analyzed for evidence of viral genetic material. The method of analysis, real-time polymerase chain reaction, PCR, is a small wonder of science, and, if it detects the SARS-CoV-2 virus, the diagnosis approaches a-hundred-per-cent accuracy: false positives are rare. But false negatives are another matter. The miss rate among people with a symptomatic infection is upward of twenty per cent, owing either to sampling problems (the swab didn’t pick up enough of a specimen) or a viral count too low to be detected. That miss rate is even higher during the four days or so before symptoms begin—going from a hundred per cent on the first day of an infection to sixty-seven per cent on the fourth day, according to a Johns Hopkins study. A negative test is not a guarantee that a person is infection-free.Unused capacity
To fix testing, we have to accelerate two lines of operation: test collection and test processing. The primary challenge of test collection—sticking a fifty-cent swab in someone’s nose—is last-mile logistics, which can be more intricate than most realize. You’ve got to manage people flow; it can be a challenge just to find locations where potentially infectious people can turn up without infecting others. Then there’s the flow of supplies, which involves having adequate quantities of the swabs and tubes that your particular lab requires, plus the personal protective equipment required for the staff. There’s the information flow—gathering and linking a patient’s information, the provider information, and the bar code on the specimen tube in a way that the laboratory can deal with. And there’s the financial flow—figuring out the billing system required to get reimbursed by the correct payer, which, for a particular person, could be Medicare or Medicaid, a private insurer, an employer, the state, the patient herself, or any number of other sources. Running a test-collection operation can be a nightmare for scores of reasons. You have to navigate supply shortages, neighborhoods that object to having lines of cars turn up at a pharmacy or clinic parking lot, business-insurance plans that may not cover you if you provide testing, and building owners with liability concerns. You may be unable to use your label printer and computer system if there’s no Wi-Fi in the parking-lot drive-up location you’ve picked. Processing tests is a very different enterprise. It is exacting. Most diagnostic tests are performed by putting a sample into a device and getting a result. But large-scale molecular diagnostic testing—in which segments of genetic material are read—isn’t done with off-the-shelf kits; these are laboratory-developed tests, meaning that running them is less like operating an appliance than like doing a procedure, with multiple steps requiring precision and tight controls. The basic coronavirus PCR test starts with a reduction process—a series of steps to wash the specimen from the swab, inactivate any virus present, and separate out the genetic material (both human and viral). What arrives at the lab as a six-inch specimen tube of material is reduced, by means of chemical reagents and various machines, to a few extracted drops of nucleic acids. Then comes the viral-detection phase. Enzymes and probes—special stretches of DNA—are added that, under the right conditions, recognize and bind to SARS-CoV-2 RNA. (The genome of coronaviruses is made of RNA, not DNA.) The binding of a probe triggers a reaction that creates a DNA transcription of the viral RNA template. That enables the final steps: the signalling process. The mixture is now put into a PCR machine—in essence, a tiny oven that sequentially heats and cools the mixture to precise temperatures, triggering further reactions that generate new copies of the viral genetic material. Each cycle of heating and cooling doubles the number of copies. After thirty cycles, up to a billion copies of viral DNA are produced from each strand. A separate marker in the mix recognizes the DNA and releases a fluorescent dye that can be measured by an optical device in the machine; there’s a threshold above which the test is considered positive. The result is checked by a technician and released electronically back to the test site. Although labs are constantly making improvements to this chain of steps in order to increase efficiency and accuracy, the whole process, from receiving a sample at a lab to sending a result, typically takes between six and twelve hours.A grid is the goal
To see what a functional national grid can deliver when it comes to public health, consider South Korea. It supported test collection, test processing, and the connections between them. On January 27th, when the country had seen just three confirmed COVID-19 cases, officials from Korea’s equivalents to the C.D.C. and F.D.A. held an urgent meeting with clinical laboratories and medical manufacturers, telling them to develop PCR tests for the new coronavirus spreading out of control in China, and to coördinate manufacturing swabs, reagents, and other necessary supplies. The government created an accelerated authorization process. By February 4th, one lab had isolated viral specimens from the three cases and reproduced the genetic material from them. Government scientists had varying dilutions put into test plates and delivered to participating laboratories as a kind of final exam for their molecular tests. If a laboratory correctly identified all the positives and negatives, its test was approved. By February 6th, the South Korean government had validated and approved tests from forty-six laboratories. Afterward, it carried out periodic cross-checks to make sure that testing remained accurate. At the same time, the government coördinated with hospitals, clinics, and public-health agencies to set up test sites, agreeing to cover the testing costs for patients (at a flat rate of sixty-seven dollars a test), and creating a common scheduling system. (Dial 1339 from anywhere in the country and you can schedule a test nearby that day.) That scheduling system also allowed them to balance the testing loads, connecting laboratories that had extra capacity to test sites where that capacity was needed. Today, South Korea, with as many people as Florida and Texas combined, has some six hundred test sites, served by a hundred and eighteen authorized laboratories, with, typically, a one-day turnaround time. That’s what a grid can get you. Other countries followed South Korea’s example. We never did. In fact, the United States has stymied rather than accelerated the ability of laboratories to develop testing capacity. In the labs of my hospital system, the Mass General Brigham—as in other academic and commercial labs—scientists began developing a coronavirus test in January, concerned that the outbreak in Asia could become a danger here. But, through February, the F.D.A. authorized only the C.D.C.’s coronavirus test. On February 20th, the Department of Health and Human Services sent out an e-mail blast to labs nationwide summarizing the Administration’s policy.Innovation’s impasse
Will improvements in techniques and technologies get us out of our testing debacle? They can help a lot—but only if we fix the underlying problem we have with delivery. Consider, for instance, pooled testing, in which you combine samples from a group of people in a single tube for a test run. A negative result will clear the entire group. If a tube comes up positive, you go back to the original samples and run them individually. During the Second World War, draftees were screened for syphilis through pooled testing. The Red Cross has used the technique to screen donated blood since 1999. In May, the Chinese government used the technique to screen the entire city of Wuhan, testing more than nine million people in ten days. (Just three hundred tests came back positive.) Pooled testing is useful when you’re screening lots of healthy people for an uncommon disease and you don’t have enough testing machines or reagents. But we’ve made no commitment to setting up the systems required to physically screen large numbers of healthy people at scale—and pooling doesn’t work if you can’t collect the specimens to pool. In communities where disease rates are high, meanwhile, pooling isn’t so valuable: too many tests will come back positive, which slows the whole production line down to a crawl. Plus, the approach doesn’t do anything about bringing online unused lab capacity, which would be needed to deploy any testing strategy efficiently. Sewage testing, one type of pooled testing, has real potential as a means of cost-efficient, large-scale screening. People infected with SARS-CoV-2 shed the virus in their stool, and PCR testing of wastewater can detect the virus upward of four days before people typically obtain clinical testing. Several hundred communities have partnered with companies such as Biobot, a Boston-area startup, to monitor viral prevalence in their populations, and the C.D.C. has announced a National Wastewater Surveillance System to track the information. The technique could be especially useful when deployed in an institutional setting: for instance, to clear a nursing home or dormitory with a single daily PCR test. The University of Arizona prevented an outbreak when regular testing of sewage samples from twenty campus buildings turned up traces of the virus from a dormitory; swab-testing the three hundred and eleven residents the next day identified two with infections. The lower limit of detection still needs to be confirmed, but Biobot claims its system can pick up a single case in up to sixty-five-hundred people. And it’s comparatively cheap: the primary cost is installing a twenty-four-hour sampling system into a building’s wastewater outflow. But, again, the mere existence of the capability is not enough. Coördinated efforts and investment are required to deploy it. The supply of compositors, the sampling devices required, must be secured. And then you need a system to provide swift follow-up testing of individuals when a sewage test comes back positive. What about at-home test collection? The F.D.A. has authorized a small number of companies—for example, LabCorp and the startup Everlywell—to give people home collection kits with specific, preapproved instructions for swabbing themselves or providing a saliva sample. Unsupervised self-collection can result in higher rates of missed infections, to be sure. And delivering and returning the tests by mail can add a couple of days to the testing process—although, as more labs gain approval for unsupervised collection kits, one can imagine pharmacies, workplaces, and schools facilitating pickup and drop-off sites that could speed it up. If we haven’t addressed the demand-capacity mismatch, however, the approach could still be slowed by lab-processing backups. You could circumvent the lab bottleneck by means of tabletop “point of care” machines that can run SARS-CoV-2 tests in clinics and other authorized settings without specialized personnel. They’re a marvel of miniaturization—akin to having your own electric generator. The White House uses these devices to test staff and visitors. There are versions that can run a PCR test in less than forty-five minutes. For those who have the money, such machines provide a means to buy your way around our broken system. But demand for the devices and the cartridges they require has far outpaced manufacturing capacity. Because each tabletop device can typically run only one sample at a time, the technology is at best a partial solution for getting to the millions of low-cost tests we need per day—there’s a difference between a Xerox machine and a printing plant. To deploy these devices, the country would still need a focussed national effort to boost the supply and get it to the populations that most need them. A cheaper type of point-of-care test has emerged that takes just fifteen minutes. Unlike PCR tests, which detect the virus’s nucleic acids, this is an “antigen” test, which detects the virus’s proteins. Most involve machines. But the Abbott antigen test card, which has just come on the market, uses the same technology as home pregnancy tests and costs labs just five dollars. It embeds a filter-paper-like strip with antibodies that trigger the release of a dye and make a line appear when they recognize and bind to SARS-CoV-2 proteins. The test is said to be almost as sensitive as PCR tests, but it has only been formally tested with (and authorized for) symptomatic patients. For people without symptoms, antigen tests are significantly less sensitive. The Abbott test card is still complex enough that it requires laboratory certification and a trained health-care worker to use it. But, with no machine needed, it’s easier to manufacture these tests at scale. The federal government has committed to buying a hundred and fifty million of these tests. How they’ll be distributed is unknown, however. With no grid to monitor need and link it with supply, distribution in this Administration has been left to the vagaries of political favor.The San Francisco model
There are places in the country that have recognized that reality. San Francisco, one of the first American cities to be hit by the pandemic, has also been one of the best at curbing it. A big reason was Mayor London Breed’s decision, starting on March 6th, less than twenty-four hours after seeing the city’s first two confirmed cases, to back the aggressive recommendations of her city’s public-health director, Grant Colfax, to halt large gatherings, suspend nonessential travel, explore work-from-home options, and rapidly deploy a citywide testing program that remains one of the country’s most effective. San Francisco’s leaders recognized the importance of universally available testing; residents needed to have an easy way to get tested regardless of what insurance they had or didn’t have, regardless of what relationship they had or didn’t have with a clinic, and regardless of whether or not they had a doctor’s order. The city’s hospitals, labs, and clinics were not going to meet that need, because that isn’t their job. In America, health-care systems are responsible for the care of individuals, not communities. So the city’s public-health department decided to step in. It took an approach that resembles South Korea’s. Officials worked with local providers and laboratories to establish a network of free drive-through and walk-in sites, open to anyone who lives or works in the city. The city established a scheduling system, which people could access online or by phone, and outreach testing for nursing homes and other vulnerable communities. Public-health officers signed standing orders for each site, eliminating the need for a doctor’s referral. The city negotiated and paid most test costs. And officials made sure that they could enlist a network of labs to provide adequate capacity and keep turnaround time low. They established, in effect, a public option for testing. Although there are scores of other test sites provided by hospitals, clinics, and pharmacies across the city, the CityTest SF network has accounted for two-thirds of the city’s daily volume of tests. The program has literally been a lifesaver. Elsewhere in California, places like Los Angeles have exploded with COVID-19 cases. San Francisco has kept the coronavirus contained. All this, alas, makes San Francisco an anomaly. Historically, the work of public health has been separate from the work of health-care delivery, using measures outside the medical system to address controllable diseases like cholera, tuberculosis, and food poisoning. But even before the coronavirus crisis hit, the separation was making less and less sense. A wide range of diseases are now controllable with the modern tools of diagnostic testing, treatment, and prevention. As the coronavirus pandemic has demonstrated, the population-level distribution of medical tests, ventilators, and drugs matters as much to disease control as nonmedical measures such as masks and social distancing. Success requires integrating the systems focussed on individual care and those focussed on community needs. We’ve long resisted that integration, though. The clearest indication is how we’ve spent our money. Spending per person on medical care was seventy-nine hundred dollars per American in 2008; it climbed to an estimated eleven thousand six hundred dollars in 2019. By contrast, the average spending per person allocated to state and local health departments was a measly eighty dollars per person in 2008, and fell to fifty-six dollars in 2019. Public-health agencies that are supposed to look after communities’ health have been forced to expand tattoo-parlor inspections while shrinking their programs to assure adequate maternal- and child-health services or screen for chronic illnesses like high blood pressure and diabetes. Talk to city and state officials about what San Francisco accomplished, and you typically hear: “Just can’t do it.” So how has San Francisco been able to pull it off? In part, it’s because the last deadly pandemic it experienced—the H.I.V./AIDS crisis—taught the city that public health and medical care must work together. San Francisco has been a pioneer in guaranteeing that H.I.V. testing and treatment is readily available and affordable to all residents in need. Those reflexes, and the associated budgeting commitment, served the city well when the coronavirus arrived. Some cities and even states—including Los Angeles, Illinois, Maine, and Tennessee—have created versions of San Francisco’s free coronavirus-testing model; the federal government set up test sites, too. Those sites received large numbers of people. But most programs don’t have sufficient funding to open enough sites—Illinois has only eleven, for instance—and the federal government opened just forty-one locations nationwide, most of which it shut down by the end of June, despite the accelerating spread of the disease. Some cities and states have run testing “blitzes,” providing public-sponsored, pop-up testing sites for a few days, with no scheduling required. But, again, because there isn’t the funding to open enough sites, lines are typically long. As cases spiked in July, almost a thousand people waited up to thirteen hours at such a site in Phoenix. Nor have these states created a system to shift testing loads to labs with capacity the way San Francisco did.Reclaiming public health
President Trump, backed by the Republican politicians who have protected him, is clearly uninterested in pursuing such goals. But even the most committed Administration would have struggled to overcome the effects of the long, collective neglect of our public-health systems. Hospitals and clinics have had the resources to spend tens of billions of dollars installing electronic medical-record systems. A whole industry has developed to deliver such capabilities. Yet our thinly staffed public-health departments, which are expected to compile thousands of diagnostic-test results per day and follow up on outbreaks, have nothing of the kind. Some still receive test results by fax and must manually enter them into databases. They lack the means to readily measure, let alone manage, a community’s availability of coronavirus tests, ventilators, hospital beds, or personal protective equipment. Not a single state in the country reports coronavirus-test turnaround time and rates of mask wearing—two of our most critical indicators for shutting the virus down. They’d like to; they just don’t have the ability to collect the information. The pandemic has given us all a master class on infectious disease, diagnostics, and the reality that individual health is inseparable from community health. Polling shows that an overwhelming majority of Americans want the government to cover the costs of not only testing but also treatment for the coronavirus. In turn, support has grown for expanding Medicare to cover all Americans for their medical needs, and for investment in public health. Epidemiologists expect us to encounter one of the worst falls and winters in American history. We will have more American dead in a single year from the pandemic than we saw during any year of war we’ve faced. On Election Day, we’ll have a chance to turn out a President who has sacrificed tens of thousands of American lives—and undermined essential government institutions—to serve his own desires. And yet, amid the carnage, there’s a lot we can still do to advance the essential work of collaboration. In New England, for example, the Assurance Testing Alliance (of which I am a founder) has been assembling a logistics grid that links schools, nursing homes, and other institutions that need regular testing to those who have the capacity to deliver it. Already, the alliance has pushed the total cost of a PCR test to fifty dollars, with a next-day turnaround time. And, beginning in August, and catalyzed by a Rockefeller Foundation effort, ten governors (so far) have formed an interstate compact to purchase and distribute enough rapid-testing devices and supplies for the delivery of five million tests. This compact enables what you’d think the United States government was created to provide: a confederation of states working to meet their common needs. Participating states share and coördinate their testing capacity, rather than bidding against one another, as they did in order to procure scarce ventilators and P.P.E. earlier in the pandemic. Alternative infrastructures like this will prove all the more important if Trump continues to control the federal government. Such efforts aren’t a replacement for national leadership, but they start the work that must be done to make ordinary physical interaction safe again, and to begin creating the public-health system we deserve. As the former Surgeon General C. Everett Koop once said, “Health care is vital to all of us some of the time, but public health is vital to all of us all of the time.” The pandemic has brought Americans a further lesson: our best chance for long, flourishing lives in the future requires that we build the foundations of our public health now. UPDATE: June 17, 2020
On March 12, our local school district closed its doors after a fifth presumed case of coronavirus was detected in our Boston suburb of 28,000. At the time, 108 total cases had been identified in Massachusetts. No deaths had yet occurred. The US totals were 1,630 cases and 41 deaths (31 of which had occurred in Washington.) Within the next week, most Massachusetts businesses and schools had been shut down.
Three months later, Massachusetts has reached 105,885 cases and 7,665 deaths. We see another 300-500 new cases and 40-50 new deaths every day. US cases are increasing at a rate of 20-25,000 per day and total over 1,225,000 – more than the next 4 countries on the list combined. About 1,000 lives are lost every day for a total of 120,000.
UPDATE: June 17, 2020
On March 12, our local school district closed its doors after a fifth presumed case of coronavirus was detected in our Boston suburb of 28,000. At the time, 108 total cases had been identified in Massachusetts. No deaths had yet occurred. The US totals were 1,630 cases and 41 deaths (31 of which had occurred in Washington.) Within the next week, most Massachusetts businesses and schools had been shut down.
Three months later, Massachusetts has reached 105,885 cases and 7,665 deaths. We see another 300-500 new cases and 40-50 new deaths every day. US cases are increasing at a rate of 20-25,000 per day and total over 1,225,000 – more than the next 4 countries on the list combined. About 1,000 lives are lost every day for a total of 120,000.
 Three months later, most businesses have reopened in Massachusetts and around the country. Wearing masks is passé, especially if you’re under 50 or a Republican. The administration insists there won’t be a second wave – that it’s just the media trying to scare people (but, sign a waiver if you’re attending one of their rallies, just in case.)
If 1,630 cases and 41 deaths were enough to essentially close down the entire country, why are the politicians and titans of finance so excited about opening it up with 1,225,000 cases and 120,000 deaths?
UPDATE: June 12, 2020
With little public discussion or debate, the US has embarked on a herd immunity approach to the coronavirus. No one’s really describing it as such, but the label is accurate just the same. Over the past month, scores of politicians and business leaders have declared (from the safety of their home offices) that “getting back to work” is more important than saving the maximum number of lives from COVID-19.
Three months later, most businesses have reopened in Massachusetts and around the country. Wearing masks is passé, especially if you’re under 50 or a Republican. The administration insists there won’t be a second wave – that it’s just the media trying to scare people (but, sign a waiver if you’re attending one of their rallies, just in case.)
If 1,630 cases and 41 deaths were enough to essentially close down the entire country, why are the politicians and titans of finance so excited about opening it up with 1,225,000 cases and 120,000 deaths?
UPDATE: June 12, 2020
With little public discussion or debate, the US has embarked on a herd immunity approach to the coronavirus. No one’s really describing it as such, but the label is accurate just the same. Over the past month, scores of politicians and business leaders have declared (from the safety of their home offices) that “getting back to work” is more important than saving the maximum number of lives from COVID-19.
 “We cannot let the cure be worse than the problem itself” tweeted President Trump. Before long, supporters appeared in statehouses across the country, sometimes toting weapons and often without masks or social distancing, protesting states’ shutdown orders and demanding their right to return to work, frequent their favorite restaurant, or host a pool party.
How most of us feel about this probably depends on their health, wealth or politics. Some consider reopening the country an economic and civil rights imperative that justifies the risk. While others, particularly those in front line jobs who can’t obtain or live on unemployment insurance, have little choice but to return to work, regardless of the risks involved. Many health care workers who have lived through the hell of a local outbreak are alarmed.
As one governor after another caved to the protestors and economic pressures, the nation held its breath. Would there be a resurgence in cases? Would areas which hadn’t previously experienced serious outbreaks be affected?
Now that all 50 states have reopened to at least some extent, the answer is clear: there has been a resurgence of cases, particularly in those states that took fewer precautions in the early days of the pandemic, closed down late, or opened up early.
“We cannot let the cure be worse than the problem itself” tweeted President Trump. Before long, supporters appeared in statehouses across the country, sometimes toting weapons and often without masks or social distancing, protesting states’ shutdown orders and demanding their right to return to work, frequent their favorite restaurant, or host a pool party.
How most of us feel about this probably depends on their health, wealth or politics. Some consider reopening the country an economic and civil rights imperative that justifies the risk. While others, particularly those in front line jobs who can’t obtain or live on unemployment insurance, have little choice but to return to work, regardless of the risks involved. Many health care workers who have lived through the hell of a local outbreak are alarmed.
As one governor after another caved to the protestors and economic pressures, the nation held its breath. Would there be a resurgence in cases? Would areas which hadn’t previously experienced serious outbreaks be affected?
Now that all 50 states have reopened to at least some extent, the answer is clear: there has been a resurgence of cases, particularly in those states that took fewer precautions in the early days of the pandemic, closed down late, or opened up early. Some states such as Washington, Vermont and Alaska, which had early success in limiting spread, are now seeing a resurgence. Others such as North Carolina, California, Texas and Arizona, which had been relatively unaffected a month or two ago, are now seeing rapid growth and new highs in cases.
Some states such as Washington, Vermont and Alaska, which had early success in limiting spread, are now seeing a resurgence. Others such as North Carolina, California, Texas and Arizona, which had been relatively unaffected a month or two ago, are now seeing rapid growth and new highs in cases.
 The implicit bet being placed is that Americans, with more money in their pockets, will ignore the rising infections and deaths in their midst.
If the numbers become too alarming, the blame can be placed on Black Lives Matter protesters instead of those protesting to reopen the country or attending political rallies.
The implicit bet being placed is that Americans, with more money in their pockets, will ignore the rising infections and deaths in their midst.
If the numbers become too alarming, the blame can be placed on Black Lives Matter protesters instead of those protesting to reopen the country or attending political rallies.
Sweden’s chief epidemiologist Anders Tegnell recently admitted that “there [was] potential for improvement in [Sweden’s herd immunity approach], quite clearly.” Asked if the country’s high death toll has made him reconsider having attempted herd immunity, Tegnell replied, “Yes, absolutely.” Looking at the continuing climb in Sweden’s new cases, it’s not hard to see why…
 …particularly when compared to its Scandinavian neighbors.
…particularly when compared to its Scandinavian neighbors.
 Two days later, I watched incredulously as she was handed a swab and told to collect her own specimen by sticking it an inch or so into her nose.
Based on what I had seen, a proper nasopharyngeal specimen requires inserting the swab several inches into someone’s nose, so far back that it reaches the back of their throat. If a person isn’t very uncomfortable, it hasn’t been done correctly.
Her results were negative but, given that the specimen wasn’t collected properly, I assumed that she could easily be one of the 30% of those who were given false negative results. It’s now a month later, and for better or worse, I’m finally beginning to believe the test results.
But, there are two important takeaways from our experience. First, the US has utterly failed in its efforts thus far. By March 8, it had conducted a total of 1,707 tests. By contrast, Italy and South Korea had each tested hundreds of thousands.
Given that up to 50-60% of all infections are asymptomatic, how many of the current 1,350,000 known cases (1,035,000 of which are still active), 166,000 of whom were hospitalized and 80,000 of whom died could have been spared had widespread testing and contract tracing been more widely available?
My daughter had a persistent cough and arrived from a country with the second highest number of infections in the world, yet no one even jotted her name down for follow up. Nor was she able to get tested until 34 days later – 36 days after Trump insisted tests were available to anybody who wanted one.
The day she returned home, China led the world with 80,735 reported cases. Italy and South Korea were in a close race for second and the US was far behind. Two months later, the US is very far ahead of the others on both an absolute and relative basis. According to experts, US cases could be 10-20 times greater as the shortage of available testing has contributed to a significant undercount.
Two days later, I watched incredulously as she was handed a swab and told to collect her own specimen by sticking it an inch or so into her nose.
Based on what I had seen, a proper nasopharyngeal specimen requires inserting the swab several inches into someone’s nose, so far back that it reaches the back of their throat. If a person isn’t very uncomfortable, it hasn’t been done correctly.
Her results were negative but, given that the specimen wasn’t collected properly, I assumed that she could easily be one of the 30% of those who were given false negative results. It’s now a month later, and for better or worse, I’m finally beginning to believe the test results.
But, there are two important takeaways from our experience. First, the US has utterly failed in its efforts thus far. By March 8, it had conducted a total of 1,707 tests. By contrast, Italy and South Korea had each tested hundreds of thousands.
Given that up to 50-60% of all infections are asymptomatic, how many of the current 1,350,000 known cases (1,035,000 of which are still active), 166,000 of whom were hospitalized and 80,000 of whom died could have been spared had widespread testing and contract tracing been more widely available?
My daughter had a persistent cough and arrived from a country with the second highest number of infections in the world, yet no one even jotted her name down for follow up. Nor was she able to get tested until 34 days later – 36 days after Trump insisted tests were available to anybody who wanted one.
The day she returned home, China led the world with 80,735 reported cases. Italy and South Korea were in a close race for second and the US was far behind. Two months later, the US is very far ahead of the others on both an absolute and relative basis. According to experts, US cases could be 10-20 times greater as the shortage of available testing has contributed to a significant undercount.
 Likewise, deaths in the US have multiplied much more rapidly than in Italy or South Korea.
Likewise, deaths in the US have multiplied much more rapidly than in Italy or South Korea.
 On both an absolute and population-weighted basis, South Korea’s aggressive testing, tracking, and quarantining measures have made a huge difference with 212 cases and 5 deaths respectively per million citizens. There have been many days over the past two weeks when South Korea reported no new cases and no new deaths.
On both an absolute and population-weighted basis, South Korea’s aggressive testing, tracking, and quarantining measures have made a huge difference with 212 cases and 5 deaths respectively per million citizens. There have been many days over the past two weeks when South Korea reported no new cases and no new deaths.
 There is some good news related to flattening the curve. The daily rate of growth in US cases and deaths continues to slow. The 10-day moving average is about 2.5% for cases and 3% for deaths. At this rate, cases will reach 1,500,000 around May 14 and deaths will reach 100,000 around May 18.
Global cases should reach the 5 million milestone by May 20 and deaths should reach 300,000 by May 14. Of course, the progression of global cases will depend largely on the US’ success or lack thereof in reopening the country.
Much has been discussed about the tradeoffs between saving the economy and saving lives. I’m neither a philosopher nor a religious scholar, so I won’t wade into the moral argument. I am troubled, however, by much of what I hear on the economic front.
To a family struggling to buy groceries or pay the rent, reopening the country is a matter of necessity rather than choice. Through no fault of their own, they must bear the economic brunt of their government’s failure to act in a timely manner to forestall the epidemic.
For many, working from home is not an option and buying groceries means exposing oneself and one’s family to serious illness and death. One particular story caught my eye this past week.
There is some good news related to flattening the curve. The daily rate of growth in US cases and deaths continues to slow. The 10-day moving average is about 2.5% for cases and 3% for deaths. At this rate, cases will reach 1,500,000 around May 14 and deaths will reach 100,000 around May 18.
Global cases should reach the 5 million milestone by May 20 and deaths should reach 300,000 by May 14. Of course, the progression of global cases will depend largely on the US’ success or lack thereof in reopening the country.
Much has been discussed about the tradeoffs between saving the economy and saving lives. I’m neither a philosopher nor a religious scholar, so I won’t wade into the moral argument. I am troubled, however, by much of what I hear on the economic front.
To a family struggling to buy groceries or pay the rent, reopening the country is a matter of necessity rather than choice. Through no fault of their own, they must bear the economic brunt of their government’s failure to act in a timely manner to forestall the epidemic.
For many, working from home is not an option and buying groceries means exposing oneself and one’s family to serious illness and death. One particular story caught my eye this past week.
 Sixty-four year-old Rafael Benjamin worked at a Cargill meat-processing plant in Pennsylvania. Many of his coworkers were falling ill, so on March 25 a daughter gave him a face mask to wear at work. Two days later, a supervisor ordered him to remove it as it made other plant employees nervous. On April 4, Rafael called in sick. The following day, unable to move, he was taken by ambulance to the hospital. He died on April 19.
On April 24, President Trump classified meat plants as critical infrastructure, preventing local and state health authorities from closing them down regardless of health concerns. The business community is working with the White House and Congress to protect companies like Cargill from customer and employee lawsuits related to coronavirus.
If passed, such legislation would allow bad actors to pressure workers to report to work regardless of their health conditions and without providing common sense safeguards. Because it would ultimately result in more illness and death, it would ironically apply additional economic pressures on the very companies seeking liability protection.
Another industry singled out for special treatment is the oil industry. If the White House and Congress were primarily concerned with unemployment in the sector, they could more vigorously subsidize payrolls instead of artificially driving the price of oil and gas higher. First, artificial price support will do nothing to correct the imbalance between supply and demand. Second, higher fuel prices are a regressive tax on those who can least afford them.
As a disciple of the Cynical School of Economic Thought, I find the entreaties by many major corporations and billionaires (most of which have cheap, ready access to capital markets) to reopen the country now to be self-serving — focused more on inflating excessive equity valuations than ensuring full employment and economic well-being for society’s most vulnerable.
Perhaps quantitative easing and financial engineering have become so effective that the economic well-being of ordinary citizens is no longer relevant. Things certainly seem to be headed in that direction.
UPDATE: Apr 17, 2020
Word on the street is that the remdesivir story was planted by a rumor-for-hire outfit and that the drug has failed in previous trials in China. Gilead has since walked back the hype.
The other COVID-19 story to hit the wires this morning is that Moderna received $483 million from the government to fast track its vaccine efforts. It’s great news, as is all the other vaccine research going on at an unprecedented pace. In listening to the CEO’s interview, however, it’s obvious that this, like every other vaccine being developed, won’t be widely available until 2021.
I’m as hopeful as anyone else. But, in the absence of a therapeutic or vaccine, I believe opening the country back up will absolutely result in a resurgence of community transmission and a sharp rise in the number of deaths – particularly in those parts of the country which have yet to be affected in great numbers.
The problem continues to be testing. If all of us pack in to a basketball game or concert and even one of us is infected, many of us will become infected. We’ll then head home and infect our loved ones and go in to the office and infect our coworkers. Since 25-50% of infected people have little or no symptoms, there is absolutely no way to prevent this from happening unless we get a vaccine.
In the US, only 13% of the 680,000 diagnosed cases have been closed – meaning either a person got better or died. Of those which were closed, nearly 40% resulted in someone dying – 34,700 of them.
Sixty-four year-old Rafael Benjamin worked at a Cargill meat-processing plant in Pennsylvania. Many of his coworkers were falling ill, so on March 25 a daughter gave him a face mask to wear at work. Two days later, a supervisor ordered him to remove it as it made other plant employees nervous. On April 4, Rafael called in sick. The following day, unable to move, he was taken by ambulance to the hospital. He died on April 19.
On April 24, President Trump classified meat plants as critical infrastructure, preventing local and state health authorities from closing them down regardless of health concerns. The business community is working with the White House and Congress to protect companies like Cargill from customer and employee lawsuits related to coronavirus.
If passed, such legislation would allow bad actors to pressure workers to report to work regardless of their health conditions and without providing common sense safeguards. Because it would ultimately result in more illness and death, it would ironically apply additional economic pressures on the very companies seeking liability protection.
Another industry singled out for special treatment is the oil industry. If the White House and Congress were primarily concerned with unemployment in the sector, they could more vigorously subsidize payrolls instead of artificially driving the price of oil and gas higher. First, artificial price support will do nothing to correct the imbalance between supply and demand. Second, higher fuel prices are a regressive tax on those who can least afford them.
As a disciple of the Cynical School of Economic Thought, I find the entreaties by many major corporations and billionaires (most of which have cheap, ready access to capital markets) to reopen the country now to be self-serving — focused more on inflating excessive equity valuations than ensuring full employment and economic well-being for society’s most vulnerable.
Perhaps quantitative easing and financial engineering have become so effective that the economic well-being of ordinary citizens is no longer relevant. Things certainly seem to be headed in that direction.
UPDATE: Apr 17, 2020
Word on the street is that the remdesivir story was planted by a rumor-for-hire outfit and that the drug has failed in previous trials in China. Gilead has since walked back the hype.
The other COVID-19 story to hit the wires this morning is that Moderna received $483 million from the government to fast track its vaccine efforts. It’s great news, as is all the other vaccine research going on at an unprecedented pace. In listening to the CEO’s interview, however, it’s obvious that this, like every other vaccine being developed, won’t be widely available until 2021.
I’m as hopeful as anyone else. But, in the absence of a therapeutic or vaccine, I believe opening the country back up will absolutely result in a resurgence of community transmission and a sharp rise in the number of deaths – particularly in those parts of the country which have yet to be affected in great numbers.
The problem continues to be testing. If all of us pack in to a basketball game or concert and even one of us is infected, many of us will become infected. We’ll then head home and infect our loved ones and go in to the office and infect our coworkers. Since 25-50% of infected people have little or no symptoms, there is absolutely no way to prevent this from happening unless we get a vaccine.
In the US, only 13% of the 680,000 diagnosed cases have been closed – meaning either a person got better or died. Of those which were closed, nearly 40% resulted in someone dying – 34,700 of them. The chart below shows that the death rate (the orange line) has remained very steady since March 26, bouncing back and forth between 35% and 43%. This is not progress, and it hardly argues for easing up on efforts to prevent community transmission.
The chart below shows that the death rate (the orange line) has remained very steady since March 26, bouncing back and forth between 35% and 43%. This is not progress, and it hardly argues for easing up on efforts to prevent community transmission.
 The US remains in 44th place in the world in testing per 1mm people. The chart below, sorted by tests per 1mm, shows some of the countries which have done much more. Not a great argument for opening up the country. The raw number of tests, BTW, is irrelevant.
The US remains in 44th place in the world in testing per 1mm people. The chart below, sorted by tests per 1mm, shows some of the countries which have done much more. Not a great argument for opening up the country. The raw number of tests, BTW, is irrelevant.  In total cases per 1mm population, the US is in 20th place…
In total cases per 1mm population, the US is in 20th place…
 …while in deaths per 1mm, the US is in 14th place. Again, not a great argument for opening up the country.
…while in deaths per 1mm, the US is in 14th place. Again, not a great argument for opening up the country.  We have had periodic declines in new deaths and cases and the rate of growth in each has definitely subsided. But, both are still occurring at an alarming rate.
We have had periodic declines in new deaths and cases and the rate of growth in each has definitely subsided. But, both are still occurring at an alarming rate.
 If the proportions hold, 1,500 of the 30,000 people diagnosed today will die — and that’s without opening up the country.
Compare the data to a country such as Germany, which imposed a stronger quarantine much earlier than the US. Sixty-two percent of all diagnosed cases have been closed, and deaths account for a mere 4% of those. Remember, the US is running about 40%.
If the proportions hold, 1,500 of the 30,000 people diagnosed today will die — and that’s without opening up the country.
Compare the data to a country such as Germany, which imposed a stronger quarantine much earlier than the US. Sixty-two percent of all diagnosed cases have been closed, and deaths account for a mere 4% of those. Remember, the US is running about 40%.
 Even though active cases have clearly rolled over…
Even though active cases have clearly rolled over…  …Germany is still seeing 3,000 new cases per day…
…Germany is still seeing 3,000 new cases per day…  …and deaths are still ticking higher.
…and deaths are still ticking higher. By comparison, the number of active cases in the US is beginning to flatten, but is far from rolling over.
By comparison, the number of active cases in the US is beginning to flatten, but is far from rolling over.
 The most frightening report I’ve seen in the past week was this one from the UN which reveals that 74 million people in the Arab region lack access to a basic handwashing facility (i.e. clean running water.) It’s safe to say that most of those 74 million also don’t have a bottle of Purell handy.
Consider the 1.2 billion people in Africa who have been so susceptible to past epidemics which were much easier to detect. The 2013-2016 Ebola outbreak in West Africa infected 28,646 and killed 11,323. Almost 20,000 cases of COVID-19 have been detected so far, and it’s still early days.
I give President Trump’s political advisors credit for convincing him to give governors the responsibility for deciding when/how to reopen their states. Those who are aggressive about it will pay the price, while those who don’t reopen things quickly will continue to pay an enormous financial price. Without widespread testing and an effective therapeutic/vaccine very soon, there will be no happy ending for either.
UPDATE: Apr 13, 2020
I’ll start with the bad news, just to change things up. The US now has almost 600,000 cases, 1 out of every 587 people and almost as many as the next 4 countries combined. Deaths, now 3.9% of all diagnosed cases, total over 23,000. Sadly, 40% of all closed cases result in someone dying.
The most frightening report I’ve seen in the past week was this one from the UN which reveals that 74 million people in the Arab region lack access to a basic handwashing facility (i.e. clean running water.) It’s safe to say that most of those 74 million also don’t have a bottle of Purell handy.
Consider the 1.2 billion people in Africa who have been so susceptible to past epidemics which were much easier to detect. The 2013-2016 Ebola outbreak in West Africa infected 28,646 and killed 11,323. Almost 20,000 cases of COVID-19 have been detected so far, and it’s still early days.
I give President Trump’s political advisors credit for convincing him to give governors the responsibility for deciding when/how to reopen their states. Those who are aggressive about it will pay the price, while those who don’t reopen things quickly will continue to pay an enormous financial price. Without widespread testing and an effective therapeutic/vaccine very soon, there will be no happy ending for either.
UPDATE: Apr 13, 2020
I’ll start with the bad news, just to change things up. The US now has almost 600,000 cases, 1 out of every 587 people and almost as many as the next 4 countries combined. Deaths, now 3.9% of all diagnosed cases, total over 23,000. Sadly, 40% of all closed cases result in someone dying.
 Fatal outcomes now account for 4% of all diagnosed cases. Another way of looking at it: for every 100 people who have been diagnosed, 90 are still sick. Of the remaining ten, 6 recovered and 4 died. Were these percentages to hold, we might expect the 26,641 new cases diagnosed just today to result in 1,065 deaths.
Fatal outcomes now account for 4% of all diagnosed cases. Another way of looking at it: for every 100 people who have been diagnosed, 90 are still sick. Of the remaining ten, 6 recovered and 4 died. Were these percentages to hold, we might expect the 26,641 new cases diagnosed just today to result in 1,065 deaths.
 But, since deaths lag new diagnoses, it would be 4% of a larger number. And, since the mortality rate is climbing every day (it was 1.2% on March 22) it would probably be a larger percentage of a larger number of people. If one of those were a friend or relative, you’d might disagree with opening up the country just yet – regardless of the trends.
Many countries have had much better outcomes, such as Switzerland where deaths are only 7% of closed cases and testing has been conducted on 22,993 per million citizens versus 8,816 per million (43rd in the world) in the US. Even Italy, to which the US is often compared, has tested 17,315 per million.
Now, for the good news. The daily rate of growth (ROG) in cases has slowed significantly – presumably as a result of quarantining (aka social distancing.) The 10-day moving average for case growth has slowed from 15% a week ago to about 10%. The 10-day moving average for the daily ROG in deaths has slowed from 22% to about 14%.
But, since deaths lag new diagnoses, it would be 4% of a larger number. And, since the mortality rate is climbing every day (it was 1.2% on March 22) it would probably be a larger percentage of a larger number of people. If one of those were a friend or relative, you’d might disagree with opening up the country just yet – regardless of the trends.
Many countries have had much better outcomes, such as Switzerland where deaths are only 7% of closed cases and testing has been conducted on 22,993 per million citizens versus 8,816 per million (43rd in the world) in the US. Even Italy, to which the US is often compared, has tested 17,315 per million.
Now, for the good news. The daily rate of growth (ROG) in cases has slowed significantly – presumably as a result of quarantining (aka social distancing.) The 10-day moving average for case growth has slowed from 15% a week ago to about 10%. The 10-day moving average for the daily ROG in deaths has slowed from 22% to about 14%.
 More testing and continued quarantining should continue to bring the growth rates down. Opening up the country without more testing, however, will only serve to increase them. At a ROG of 14%, deaths will reach 100,000 by April 24. Slowing the rate to 10% (i.e. flattening the curve) would delay that milestone to Apr 28 and to 5% would delay it to May 13. This would buy scientists more time to come up with effective therapeutics.
Getting tested? It’s easier now but, based on my experience, not very accurate. I took my daughter (who returned from Italy with a bad cough) to a drive-through testing site run by CVS. It was fast and free, but they handed my daughter the swab and asked her to collect her own specimen.
She inserted the swab about 1 – 1.5 inches into each nostril, at which point the tech said “good job” and put the sample into a bag for assessment. This was completely inadequate and is probably responsible for the 30%+ false negative results being obtained.
An accurate nasopharyngeal specimen collection means sticking the swab so far back that most people would gag and tear up in the process. Here’s a video of the correct process. Bottom line, don’t assume that a negative test is correct. Continue to exercise caution – particularly if someone is exhibiting symptoms.
More testing and continued quarantining should continue to bring the growth rates down. Opening up the country without more testing, however, will only serve to increase them. At a ROG of 14%, deaths will reach 100,000 by April 24. Slowing the rate to 10% (i.e. flattening the curve) would delay that milestone to Apr 28 and to 5% would delay it to May 13. This would buy scientists more time to come up with effective therapeutics.
Getting tested? It’s easier now but, based on my experience, not very accurate. I took my daughter (who returned from Italy with a bad cough) to a drive-through testing site run by CVS. It was fast and free, but they handed my daughter the swab and asked her to collect her own specimen.
She inserted the swab about 1 – 1.5 inches into each nostril, at which point the tech said “good job” and put the sample into a bag for assessment. This was completely inadequate and is probably responsible for the 30%+ false negative results being obtained.
An accurate nasopharyngeal specimen collection means sticking the swab so far back that most people would gag and tear up in the process. Here’s a video of the correct process. Bottom line, don’t assume that a negative test is correct. Continue to exercise caution – particularly if someone is exhibiting symptoms.
 And, even if some politician gives you the all clear, remember that nearly 30,000 new cases will be diagnosed today. Don’t be one of them.
UPDATE: April 3, 2020
Out of curiosity, I took a look at mortality rate trends in a few other countries. While some are clearly better than others, every single one is rising consistently over the past week.
And, even if some politician gives you the all clear, remember that nearly 30,000 new cases will be diagnosed today. Don’t be one of them.
UPDATE: April 3, 2020
Out of curiosity, I took a look at mortality rate trends in a few other countries. While some are clearly better than others, every single one is rising consistently over the past week.
 And, deaths are consistently rising faster than cases. Cases have risen an average of 2x over the past week, while deaths have risen an average of 3.4x. In the US, the numbers are 2.9x and 4.7x – a ratio of 1.64 deaths per every new case diagnosed. In Germany, deaths are rising over twice as fast as cases.
I have very little medical training, but I believe this is why we’re hearing so much about flattening the curve. The experts know that our hospitals will be overwhelmed if the ROG doesn’t slow dramatically. Overwhelmed hospitals and shortages of ICU beds and ventilators will translate into higher mortality rates.
In some cases, however, the higher mortality rate can be attributed to a drop in the rate of growth in new cases. Due to the lag between diagnosis and death, case growth can roll over as deaths are still rising. A good example is Austria. New cases peaked on March 26 while deaths peaked on March 30.
And, deaths are consistently rising faster than cases. Cases have risen an average of 2x over the past week, while deaths have risen an average of 3.4x. In the US, the numbers are 2.9x and 4.7x – a ratio of 1.64 deaths per every new case diagnosed. In Germany, deaths are rising over twice as fast as cases.
I have very little medical training, but I believe this is why we’re hearing so much about flattening the curve. The experts know that our hospitals will be overwhelmed if the ROG doesn’t slow dramatically. Overwhelmed hospitals and shortages of ICU beds and ventilators will translate into higher mortality rates.
In some cases, however, the higher mortality rate can be attributed to a drop in the rate of growth in new cases. Due to the lag between diagnosis and death, case growth can roll over as deaths are still rising. A good example is Austria. New cases peaked on March 26 while deaths peaked on March 30.

 This has allowed its mortality rate to almost flatten: from 1.3% on March 31 to only 1.5% on April 3. And, its curve is definitely flattening. Note that Austria enacted nationwide restrictions on travel and gatherings on March 16 when there were 1,018 total cases and 3 deaths. This was 18 days after the first community transmission case was detected and two days after the first death.
This has allowed its mortality rate to almost flatten: from 1.3% on March 31 to only 1.5% on April 3. And, its curve is definitely flattening. Note that Austria enacted nationwide restrictions on travel and gatherings on March 16 when there were 1,018 total cases and 3 deaths. This was 18 days after the first community transmission case was detected and two days after the first death. The US, by contrast, has still not enacted a nationwide lockdown despite over 300,000 cases and 8,000 deaths since the virus arrived over two months ago on January 20.
The US, by contrast, has still not enacted a nationwide lockdown despite over 300,000 cases and 8,000 deaths since the virus arrived over two months ago on January 20.
 The 10-day moving average of the daily rate of growth in deaths in the US dipped slightly to 27.3%. But at this rate we would still reach 10,000 deaths this weekend, 100,000 by April 14, and 1 million by April 24.
The 10-day moving average of the daily rate of growth in deaths in the US dipped slightly to 27.3%. But at this rate we would still reach 10,000 deaths this weekend, 100,000 by April 14, and 1 million by April 24.  Some might feel this rate is too pessimistic, that something will happen to change the trajectory. I hope so. But, even if the rate were to plunge to 20%, we would still have over 1 million deaths before the end of April – one in every 323 people in the US. And, remember, this number is understated – though not as dramatically as the number of cases.
Don’t wait for the government to tell you what we already know: the only way to be completely safe is to stay at home, away from anyone who might be infected (including asymptomatic family members) and to wear a mask if you absolutely must go out – especially around other people. Assume that everything you touch might harbor the virus.
Yes, you might feel like you look really paranoid. But, your family will thank you. And, God willing, you can all laugh about it some day.
For those staying in this weekend, I just read that HBO is releasing 500 hours of programming for free, including every including every episode of The Sopranos, Veep, The Wire, Barry and Ballers. You can download the HBO NOW or HBO GO apps or visit HBONOW.com or HBOGO.com. #StayHomeBoxOffice.
Stay safe everyone.
UPDATE: March 31, 2020
Italy’s mortality rate continues climbing steadily: from 2.0% on March 1 to 11.4% as of March 30. I never see this data reported anywhere, but believe it’s very important as it confirms what should be obvious: An overwhelmed health system is not as effective in saving the lives of sick COVID-19 patients.
Those in the US who take comfort in its current 2% mortality rate probably shouldn’t. Reported cases – still an understatement of actual cases due to the continuing shortage of test kits – continue to increase at an average (10-day SMA) of 24% per day. But, deaths are climbing at about 30% per day – much faster in some states. Inexplicably, many states have yet to issue stay-at-home orders.
Some might feel this rate is too pessimistic, that something will happen to change the trajectory. I hope so. But, even if the rate were to plunge to 20%, we would still have over 1 million deaths before the end of April – one in every 323 people in the US. And, remember, this number is understated – though not as dramatically as the number of cases.
Don’t wait for the government to tell you what we already know: the only way to be completely safe is to stay at home, away from anyone who might be infected (including asymptomatic family members) and to wear a mask if you absolutely must go out – especially around other people. Assume that everything you touch might harbor the virus.
Yes, you might feel like you look really paranoid. But, your family will thank you. And, God willing, you can all laugh about it some day.
For those staying in this weekend, I just read that HBO is releasing 500 hours of programming for free, including every including every episode of The Sopranos, Veep, The Wire, Barry and Ballers. You can download the HBO NOW or HBO GO apps or visit HBONOW.com or HBOGO.com. #StayHomeBoxOffice.
Stay safe everyone.
UPDATE: March 31, 2020
Italy’s mortality rate continues climbing steadily: from 2.0% on March 1 to 11.4% as of March 30. I never see this data reported anywhere, but believe it’s very important as it confirms what should be obvious: An overwhelmed health system is not as effective in saving the lives of sick COVID-19 patients.
Those in the US who take comfort in its current 2% mortality rate probably shouldn’t. Reported cases – still an understatement of actual cases due to the continuing shortage of test kits – continue to increase at an average (10-day SMA) of 24% per day. But, deaths are climbing at about 30% per day – much faster in some states. Inexplicably, many states have yet to issue stay-at-home orders.
 The top 25 states in terms of cases are shown below. Note that Louisiana, a relative newcomer to the top 10, is already at a mortality rate of 4.6% – topping Washington’s 4%. Virginia’s governor finally issued a stay-at-home order yesterday, as that state’s mortality rate reached 2.5%.
Several cities and counties in Georgia, which faces a 3.4% mortality rate, have issued orders; but, the governor has yet to announce a statewide order. Arizona’s governor, who had issued an order restricting the ability of cities and counties to issue their own orders without his approval, finally caved yesterday when cases topped 1,000.
The top 25 states in terms of cases are shown below. Note that Louisiana, a relative newcomer to the top 10, is already at a mortality rate of 4.6% – topping Washington’s 4%. Virginia’s governor finally issued a stay-at-home order yesterday, as that state’s mortality rate reached 2.5%.
Several cities and counties in Georgia, which faces a 3.4% mortality rate, have issued orders; but, the governor has yet to announce a statewide order. Arizona’s governor, who had issued an order restricting the ability of cities and counties to issue their own orders without his approval, finally caved yesterday when cases topped 1,000.
 As more hospitals across the nation are overwhelmed by cases that outnumber the available ICU beds and ventilators, the mortality rate is bound to rise. Those that restrict transmissions before cases get out of hand stand the best chance of not being overwhelmed. The rest will suffer the consequences. As Dr. Georges Benjamin, executive director of the American Public Health Association, said: “Waiting until you get a lot of cases is the wrong strategy.”
Currently, about 1/3 of closed cases – someone being either discharged or dying – result in a death. But, only 5% of total reported cases have been closed – again, a factor of the rapid growth in cases. In Italy, where 26% of all cases have been closed, deaths account for 44% of all closed cases and, as mentioned above, 11.4% of total cases.
Applying the same percentages to US cases would indicate that 2,313 of the 20,297 new cases reported just on March 30 will result in someone dying. At the current daily rate of increase, the US will reach 10,000 deaths by April 4 and 100,000 on or around Easter. My projections indicate total cases could reach 2.4 million by then, swamping the 924,000 beds in the 5,198 community hospitals across the nation.
If even 5% of those cases were serious/critical, the resulting 120,000 cases would far outnumber the 77,000 ICU beds in the US.
As more hospitals across the nation are overwhelmed by cases that outnumber the available ICU beds and ventilators, the mortality rate is bound to rise. Those that restrict transmissions before cases get out of hand stand the best chance of not being overwhelmed. The rest will suffer the consequences. As Dr. Georges Benjamin, executive director of the American Public Health Association, said: “Waiting until you get a lot of cases is the wrong strategy.”
Currently, about 1/3 of closed cases – someone being either discharged or dying – result in a death. But, only 5% of total reported cases have been closed – again, a factor of the rapid growth in cases. In Italy, where 26% of all cases have been closed, deaths account for 44% of all closed cases and, as mentioned above, 11.4% of total cases.
Applying the same percentages to US cases would indicate that 2,313 of the 20,297 new cases reported just on March 30 will result in someone dying. At the current daily rate of increase, the US will reach 10,000 deaths by April 4 and 100,000 on or around Easter. My projections indicate total cases could reach 2.4 million by then, swamping the 924,000 beds in the 5,198 community hospitals across the nation.
If even 5% of those cases were serious/critical, the resulting 120,000 cases would far outnumber the 77,000 ICU beds in the US.
 Bloomberg pubished an interesting article earlier today citing an Italian study that offered a theory as to why Italy’s mortality rate is so high. The study suggested that because Italy had such a mild winter, many of the deaths that might ordinarily have occurred due to flu were brought on instead by the coronavirus. The inference is that the mortality rate is much higher than it would otherwise be had the winter been colder.
While I certainly find the premise plausible, it doesn’t do much to move the needle. The study suggests that “the total number of older Italians spared death directly from the flu this season may have been in the hundreds, based on an annual average of 8,000 nationwide flu deaths cited in the paper.”
Italy has seen over 12,000 deaths. Subtracting 500, for instance, would lower its mortality rate from 11.4% a still very high 10.9%. Having had a daughter in Italy between late January and March 8, I followed the situation very closely. I think the high death rate is much more likely to have been the result of some bad luck (getting hit with the first burst of infections) and a failure to lock down the entire country.
Early on, several small towns in northern Italy were quarantined. Many who were able to simply left the area, returning to their homes in southern Italy or elsewhere in Europe. As cases spread, Milan was included in the quarantine. Again, this didn’t stop anyone from returning to their home. As I wrote at the time, 20,000 people were taking a train from Milan to Rome every day.
Eventually, the entire country was put on lockdown. But, by then, the spread had occurred and quickly overwhelmed the available hospital facilities. While cases increased 59X between Mar 1 and Mar 30, deaths increased 341X.
This is why I believe a nationwide lockdown is essential for the US. We all know someone who left a heavily infected area to go someplace “safe” such as a friend or relative’s house, a second home or just a hotel. Unfortunately, some of those people are infected and transmit the disease to people in the other location. It only takes a few to get the community spread ball rolling. This is precisely what happened in Europe.
True, there are some very efficient and tightly controlled countries in Europe with low mortality rates (so far) such as Switzerland (2.7%), Austria (1.4%) and Germany (1.1%). But, each of these took early, aggressive measures to limit the spread. Many other countries are slightly behind but on the same track as Italy: France (6.8%), Spain (8.9%), UK (7.8%), and Netherlands (8.6%.)
A March 30 study from Imperial College of London researchers draws a direct correlation between the number of deaths and the speed with which various countries took steps to intervene in the virus’ spread. All but one (Sweden) ultimately ordered a lockdown – typically as each country’s leaders realized they would not be spared.
Bloomberg pubished an interesting article earlier today citing an Italian study that offered a theory as to why Italy’s mortality rate is so high. The study suggested that because Italy had such a mild winter, many of the deaths that might ordinarily have occurred due to flu were brought on instead by the coronavirus. The inference is that the mortality rate is much higher than it would otherwise be had the winter been colder.
While I certainly find the premise plausible, it doesn’t do much to move the needle. The study suggests that “the total number of older Italians spared death directly from the flu this season may have been in the hundreds, based on an annual average of 8,000 nationwide flu deaths cited in the paper.”
Italy has seen over 12,000 deaths. Subtracting 500, for instance, would lower its mortality rate from 11.4% a still very high 10.9%. Having had a daughter in Italy between late January and March 8, I followed the situation very closely. I think the high death rate is much more likely to have been the result of some bad luck (getting hit with the first burst of infections) and a failure to lock down the entire country.
Early on, several small towns in northern Italy were quarantined. Many who were able to simply left the area, returning to their homes in southern Italy or elsewhere in Europe. As cases spread, Milan was included in the quarantine. Again, this didn’t stop anyone from returning to their home. As I wrote at the time, 20,000 people were taking a train from Milan to Rome every day.
Eventually, the entire country was put on lockdown. But, by then, the spread had occurred and quickly overwhelmed the available hospital facilities. While cases increased 59X between Mar 1 and Mar 30, deaths increased 341X.
This is why I believe a nationwide lockdown is essential for the US. We all know someone who left a heavily infected area to go someplace “safe” such as a friend or relative’s house, a second home or just a hotel. Unfortunately, some of those people are infected and transmit the disease to people in the other location. It only takes a few to get the community spread ball rolling. This is precisely what happened in Europe.
True, there are some very efficient and tightly controlled countries in Europe with low mortality rates (so far) such as Switzerland (2.7%), Austria (1.4%) and Germany (1.1%). But, each of these took early, aggressive measures to limit the spread. Many other countries are slightly behind but on the same track as Italy: France (6.8%), Spain (8.9%), UK (7.8%), and Netherlands (8.6%.)
A March 30 study from Imperial College of London researchers draws a direct correlation between the number of deaths and the speed with which various countries took steps to intervene in the virus’ spread. All but one (Sweden) ultimately ordered a lockdown – typically as each country’s leaders realized they would not be spared.
 While identifying and limiting the spread of US cases is incredibly important, note that I have focused mostly on the trend in deaths — which distills all the theories and practices into one defining, indisputable and depressing number every day. It’s where the rubber meets the road.
I printed a list of the top 25 states in terms of cases as of March 30 above. Mortality rates ranged from 0.5% to 4.6% with a median of 1.7% and a mean of 1.9%.
At the end of today, March 31, the range was from 1.1% to 4.6% with a median of 2.1% and a mean of 2.2%. While total deaths grew by 31% in that one 24-hour period, the average daily rate of increase among the 25 states was a stunning 47%.
While identifying and limiting the spread of US cases is incredibly important, note that I have focused mostly on the trend in deaths — which distills all the theories and practices into one defining, indisputable and depressing number every day. It’s where the rubber meets the road.
I printed a list of the top 25 states in terms of cases as of March 30 above. Mortality rates ranged from 0.5% to 4.6% with a median of 1.7% and a mean of 1.9%.
At the end of today, March 31, the range was from 1.1% to 4.6% with a median of 2.1% and a mean of 2.2%. While total deaths grew by 31% in that one 24-hour period, the average daily rate of increase among the 25 states was a stunning 47%.
 Note that the order of the top 25 has changed. Florida has moved into the #5 slot, Illinois has moved ahead of Washington to #7, Louisiana moved from #10 to #9, Georgia moved ahead of Texas to #11, etc. I’ll continue to track these same 25 so we can stay abreast of the trend.
The important thing to realize is that deaths continue to rise sharply. As in Europe, the growth has tended to accelerate faster in states which were late to start testing, close schools and businesses, and issue stay-at-home orders. Those that have not restricted movement should expect to see deaths continue to outpace those that have.
With a total of 4,053 deaths as we goes to press, rising at a 10-day moving average of 29.8% per day, total US deaths should reach 10,000 by Saturday April 4, 100,000 by April 13, 500,000 by April 19 and 1 million by April 22.
Note that the order of the top 25 has changed. Florida has moved into the #5 slot, Illinois has moved ahead of Washington to #7, Louisiana moved from #10 to #9, Georgia moved ahead of Texas to #11, etc. I’ll continue to track these same 25 so we can stay abreast of the trend.
The important thing to realize is that deaths continue to rise sharply. As in Europe, the growth has tended to accelerate faster in states which were late to start testing, close schools and businesses, and issue stay-at-home orders. Those that have not restricted movement should expect to see deaths continue to outpace those that have.
With a total of 4,053 deaths as we goes to press, rising at a 10-day moving average of 29.8% per day, total US deaths should reach 10,000 by Saturday April 4, 100,000 by April 13, 500,000 by April 19 and 1 million by April 22.
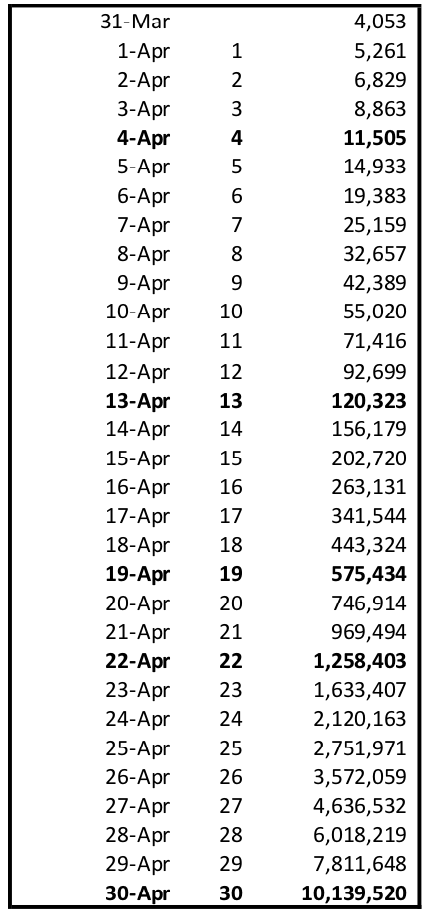 I believe that this fate can be avoided only if: (a) everyone who should be tested is tested, (b) the entire nation is locked down, and (c) scientists can develop effective treatments in the next week or so. I hope to God I’m wrong.
A few reminders that I haven’t seen circulated nearly enough: Studies indicate that up to 50% of transmissions are from people who have little or no symptoms. Your kid or your neighbor who appears perfectly healthy can give you the virus.
And, studies now indicate that the coronavirus can remain aerosolized for up to three hours. You could be walking down a deserted aisle at the grocery store and stroll right through the viral mist emitted by someone who sneezed there 20 minutes ago. Wear a mask when out in public places and assume that everything you touch is infected.
I believe that this fate can be avoided only if: (a) everyone who should be tested is tested, (b) the entire nation is locked down, and (c) scientists can develop effective treatments in the next week or so. I hope to God I’m wrong.
A few reminders that I haven’t seen circulated nearly enough: Studies indicate that up to 50% of transmissions are from people who have little or no symptoms. Your kid or your neighbor who appears perfectly healthy can give you the virus.
And, studies now indicate that the coronavirus can remain aerosolized for up to three hours. You could be walking down a deserted aisle at the grocery store and stroll right through the viral mist emitted by someone who sneezed there 20 minutes ago. Wear a mask when out in public places and assume that everything you touch is infected.
* * *
UPDATE: March 22, 2020 Italy’s mortality rate increased to 9.3% on March 22, a steady increase from 2.0% on Mar 1. Though, on a positive note, the daily rate of growth in cases and deaths has ebbed somewhat: Neither has exceeded 20% since March 13. On a not so positive note, both are still doubling every 6-7 days. The daily ROG in US deaths ticked lower on March 20-21, but pushed back up to 39% on March 22. At this rate, the 419 US deaths as of March 22 would exceed 1,000 by March 25, 10,000 by April 1, and 100,000 by April 8. Take a moment and let those numbers sink in.
The daily ROG in US deaths ticked lower on March 20-21, but pushed back up to 39% on March 22. At this rate, the 419 US deaths as of March 22 would exceed 1,000 by March 25, 10,000 by April 1, and 100,000 by April 8. Take a moment and let those numbers sink in.
 Italy still has many active cases, 80% of the total. Fortunately, most are resolving as “recovered/discharged.” But, the 9.3% mortality rate – up from only 2% on March 1 – means that nearly as many die as are discharged/recovered.
Italy still has many active cases, 80% of the total. Fortunately, most are resolving as “recovered/discharged.” But, the 9.3% mortality rate – up from only 2% on March 1 – means that nearly as many die as are discharged/recovered. Only a very small fraction of US cases are closed. Unfortunately, about 73% of closed cases have resulted in death rather than recovery.
Only a very small fraction of US cases are closed. Unfortunately, about 73% of closed cases have resulted in death rather than recovery.
 This is up from 60% of cases just 4 days ago. Serious/critical cases as a percentage of active cases have more than quadrupled in that time. In other words, things are getting worse at an accelerating rate.
This is up from 60% of cases just 4 days ago. Serious/critical cases as a percentage of active cases have more than quadrupled in that time. In other words, things are getting worse at an accelerating rate.
 I regret to report that our original models posted on March 13-14 have not kept up with the actual results. The model which used the then 10-DMAs of daily rates of growth for cases and deaths (34% and 18%) had forecast 23,410 cases and 247 deaths for March 22.
The model which borrowed the 10-DMA of Italy’s daily ROG with an 11-day lag had forecast 23,410 cases and 481 deaths.
As of last night, total acknowledged US cases totaled 33,546 (still undercounted) and deaths totaled 419.
I regret to report that our original models posted on March 13-14 have not kept up with the actual results. The model which used the then 10-DMAs of daily rates of growth for cases and deaths (34% and 18%) had forecast 23,410 cases and 247 deaths for March 22.
The model which borrowed the 10-DMA of Italy’s daily ROG with an 11-day lag had forecast 23,410 cases and 481 deaths.
As of last night, total acknowledged US cases totaled 33,546 (still undercounted) and deaths totaled 419.
* * *
UPDATE: Mar 17, 2020 For those interested, here is an update on the current case and death data for Italy and the US as of Mar 16. In Italy, the current mortality rate has ticked up even higher to 7.7%. The 10-day moving average for mortality rate has increased to 6.3%. The 10-DMA for the ROG in cases and deaths has eased slightly to 21% and 28%.| Italy | ||
| date | cases | deaths |
| 21-Feb | 21 | 1 |
| 22-Feb | 79 | 2 |
| 23-Feb | 152 | 2 |
| 24-Feb | 229 | 6 |
| 25-Feb | 322 | 11 |
| 26-Feb | 400 | 12 |
| 27-Feb | 655 | 17 |
| 28-Feb | 889 | 21 |
| 29-Feb | 1,128 | 29 |
| 1-Mar | 1,701 | 34 |
| 2-Mar | 2,036 | 52 |
| 3-Mar | 2,502 | 79 |
| 4-Mar | 3,089 | 107 |
| 5-Mar | 3,858 | 148 |
| 6-Mar | 4,636 | 197 |
| 7-Mar | 5,883 | 233 |
| 8-Mar | 7,375 | 366 |
| 9-Mar | 9,172 | 463 |
| 10-Mar | 10,149 | 631 |
| 11-Mar | 12,462 | 827 |
| 12-Mar | 15,113 | 1,016 |
| 13-Mar | 17,660 | 1,266 |
| 14-Mar | 21,157 | 1,441 |
| 15-Mar | 24,747 | 1,809 |
| 16-Mar | 27,980 | 2,158 |
| 17-Mar | ||
| 18-Mar | ||
| 19-Mar |
 The US, unfortunately, has managed to keep pace with our forecast from March 13 which was based on a moving average of growth rates. On March 13, our model predicted 5,444 cases and 80 deaths for March 16. Actual results were 4,663 cases and 86 deaths.
Again, the continuing lack of testing kits renders the number of cases essentially meaningless. Many experts feel it could be off by a factor of at least 10X, possibly much more.
The number of deaths, unfortunately, is probably accurate. The 10-DMA for daily ROG in deaths has risen from 18% on March 13 to 19.2%. The chart below reflects these data and uses the most recent 10-DMA in daily ROG for each category to forecast future results (in italics.)
The US, unfortunately, has managed to keep pace with our forecast from March 13 which was based on a moving average of growth rates. On March 13, our model predicted 5,444 cases and 80 deaths for March 16. Actual results were 4,663 cases and 86 deaths.
Again, the continuing lack of testing kits renders the number of cases essentially meaningless. Many experts feel it could be off by a factor of at least 10X, possibly much more.
The number of deaths, unfortunately, is probably accurate. The 10-DMA for daily ROG in deaths has risen from 18% on March 13 to 19.2%. The chart below reflects these data and uses the most recent 10-DMA in daily ROG for each category to forecast future results (in italics.)
| US: 10-DMA | ||
| date | cases | deaths |
| 3-Mar | 124 | 9 |
| 4-Mar | 158 | 11 |
| 5-Mar | 221 | 12 |
| 6-Mar | 319 | 15 |
| 7-Mar | 435 | 19 |
| 8-Mar | 541 | 22 |
| 9-Mar | 704 | 26 |
| 10-Mar | 994 | 30 |
| 11-Mar | 1,301 | 38 |
| 12-Mar | 1,697 | 41 |
| 13-Mar | 2,269 | 48 |
| 14-Mar | 2,943 | 57 |
| 15-Mar | 3,680 | 68 |
| 16-Mar | 4,663 | 86 |
| 17-Mar | 6,102 | 103 |
| 18-Mar | 7,984 | 122 |
| 19-Mar | 10,448 | 146 |
| 20-Mar | 13,672 | 174 |
| 21-Mar | 17,890 | 207 |
| 22-Mar | 23,410 | 247 |
| 23-Mar | 30,632 | 294 |
| 24-Mar | 40,084 | 351 |
| 25-Mar | 52,451 | 418 |
| 26-Mar | 68,635 | 499 |
| 27-Mar | 89,812 | 595 |
| 28-Mar | 117,523 | 709 |
| 29-Mar | 153,784 | 845 |
| 30-Mar | 201,232 | 1,008 |
| US: It ROG | ||
| date | cases | deaths |
| 3-Mar | 124 | 9 |
| 4-Mar | 158 | 11 |
| 5-Mar | 221 | 12 |
| 6-Mar | 319 | 15 |
| 7-Mar | 435 | 19 |
| 8-Mar | 541 | 22 |
| 9-Mar | 704 | 26 |
| 10-Mar | 994 | 30 |
| 11-Mar | 1,301 | 38 |
| 12-Mar | 1,697 | 41 |
| 13-Mar | 2,269 | 48 |
| 14-Mar | 2,943 | 57 |
| 15-Mar | 3,680 | 68 |
| 16-Mar | 4,663 | 86 |
| 17-Mar | 6,102 | 114 |
| 18-Mar | 7,984 | 135 |
| 19-Mar | 10,448 | 213 |
| 20-Mar | 13,672 | 269 |
| 21-Mar | 17,890 | 367 |
| 22-Mar | 23,410 | 481 |
| 23-Mar | 30,632 | 590 |
| 24-Mar | 40,084 | 736 |
| 25-Mar | 52,451 | 837 |
| 26-Mar | 68,635 | 1,051 |
| 27-Mar | 89,812 | 1,254 |
| 28-Mar | ||
| 29-Mar | ||
| 30-Mar |

 As in Italy, once hospital beds and ventilators are impacted the mortality rate will go up. By slowing admissions, we can reduce overcrowded conditions and keep the mortality rate lower. At least, that’s the theory.
It’s important to note that even a slight increase has a huge impact on resulting cases and deaths. The chart below shows deaths at Day 5, 10 and 30 for different daily rates of growth.
As in Italy, once hospital beds and ventilators are impacted the mortality rate will go up. By slowing admissions, we can reduce overcrowded conditions and keep the mortality rate lower. At least, that’s the theory.
It’s important to note that even a slight increase has a huge impact on resulting cases and deaths. The chart below shows deaths at Day 5, 10 and 30 for different daily rates of growth.
| ROG | Day 1 | Day 5 | Day 10 | Day 30 |
| 5% | 86 | 110 | 140 | 372 |
| 10% | 86 | 139 | 223 | 1,501 |
| 15% | 86 | 173 | 348 | 5,694 |
| 20% | 86 | 214 | 532 | 20,414 |
| 25% | 86 | 262 | 801 | 69,470 |
| 30% | 86 | 319 | 1,186 | 225,320 |
* * *
March 13, 2020 I saw something quite stunning this morning: Treasury Secretary Mnuchin describing the COVID-19 pandemic as “a great investment opportunity.” Tone deaf as ever, but no surprise there. He then went on to draw comparisons to South Korea’s experience where 200,000 people have been tested – only 4% of which were found to be infected, as though this meant there was nothing to worry about. Let’s unpack this, shall we? Actually, 222,000 people in South Korea have been tested — about .44%, or one in every 225 people. In the US, the number of people who have been tested was recently removed from the CDC website. But, many academics put it at approximately 13,600, about .0042%, or one in every 24,200 Americans. In South Korea, the government can access data – CCTV footage, GPS tracking data from phones and cars, credit cards transactions, immigration records and other data to deduce who might be at risk of contracting the disease or passing it to others. Anyone who wants testing can get it, with drive-through testing in place since March 2.
The names of those Koreans found to be infected are made public so friends and relatives who might have been exposed can get themselves tested. Anyone who tests positive is self-quarantined and monitored through an app or by phone until a bed is available, at which point an ambulance delivers them to a hospital with air-sealed isolation rooms.
In the US, an acquaintance recently told me of arriving from an extended trip to Italy and breezing through customs with a noticeable, persistent cough. No one took their temperature, asked their health status or jotted their name down for follow-up. When they called their US doctor, they were told they couldn’t be tested unless their fever topped 100.4 degrees due to a shortage of test kits. The drive-through idea was just announced today.
In South Korea, the government can access data – CCTV footage, GPS tracking data from phones and cars, credit cards transactions, immigration records and other data to deduce who might be at risk of contracting the disease or passing it to others. Anyone who wants testing can get it, with drive-through testing in place since March 2.
The names of those Koreans found to be infected are made public so friends and relatives who might have been exposed can get themselves tested. Anyone who tests positive is self-quarantined and monitored through an app or by phone until a bed is available, at which point an ambulance delivers them to a hospital with air-sealed isolation rooms.
In the US, an acquaintance recently told me of arriving from an extended trip to Italy and breezing through customs with a noticeable, persistent cough. No one took their temperature, asked their health status or jotted their name down for follow-up. When they called their US doctor, they were told they couldn’t be tested unless their fever topped 100.4 degrees due to a shortage of test kits. The drive-through idea was just announced today.
All things considered, I consider South Korea a very poor comparison. For the past several weeks, I have focused instead on Italy. Like the US, they have a modern health care system, but were caught completely off guard when COVID-19 arrived from China. Italians are also used to a certain degree of autonomy and would presumably bristle at the intrusiveness of South Korea’s response.
About 11,500 Chinese travel to Italy each day compared to 14,000 who travel to the US. The US instituted a travel ban (with some exceptions) from China on February 4. Foreigners were mostly turned away, but others had their temperature taken and were asked to self-quarantine. Italy instituted a travel ban with no exceptions, and no flights whatsoever, four days earlier.
 Italy locked down the northern part of the country, putting 16 million people on lockdown on March 8. The lockdown was extended to the entire country – 60 million people – on Tuesday, with essentially every establishment except grocery stores and pharmacies closed.
In the US, not a single city or state has been quarantined. Over the past few days, many schools, sporting events, concerts, conventions and the like have made the decision to close or operate online. I am not aware of a single enforced quarantine other than those who returned from a cruise or trip overseas and were clearly infected. Americans are asked to self-quarantine, which is fine in concept but doesn’t work very well given that the incubation period can be two weeks or longer, and few can afford to ditch their jobs for two weeks.
Italy has essentially been shut down, even though its response has arguably been much more robust than America’s. In my opinion, this doesn’t bode well for the US. I have been making predictions for the past several weeks based upon comparisons between the two: schools closing, stores closing, travel restrictions, runs on cleaning supplies and groceries. Many readers, not to mention friends and family, who initially scoffed are no longer scoffing. I get many texts and emails every day saying something along the lines of “can you believe they just cancelled…?”
I’m a numbers guy, so I’ve been working diligently to come up with a formula that expressed the path the number of cases and deaths was taking. The problem is that only a small number of cases have resolved in both Italy and the US.
Total cases in the US are (supposedly) 2,269. This is no doubt very far short of the actual number due to the lack of available testing. But, the outcome data are telling. Only 79 of these 2,269 are closed: 39% due to the patients’ recovery and 61% due to their death. This leaves 2,190 in limbo, whose fate is as yet undetermined. But, we can make some educated guesses.
While the cases are almost certainly undercounted, the number of deaths is probably fairly accurate. At 48 total deaths, the current mortality rate is 2.1%. Some might take solace in such a low number. But, that would probably be a mistake. The Italy data are below.
Italy locked down the northern part of the country, putting 16 million people on lockdown on March 8. The lockdown was extended to the entire country – 60 million people – on Tuesday, with essentially every establishment except grocery stores and pharmacies closed.
In the US, not a single city or state has been quarantined. Over the past few days, many schools, sporting events, concerts, conventions and the like have made the decision to close or operate online. I am not aware of a single enforced quarantine other than those who returned from a cruise or trip overseas and were clearly infected. Americans are asked to self-quarantine, which is fine in concept but doesn’t work very well given that the incubation period can be two weeks or longer, and few can afford to ditch their jobs for two weeks.
Italy has essentially been shut down, even though its response has arguably been much more robust than America’s. In my opinion, this doesn’t bode well for the US. I have been making predictions for the past several weeks based upon comparisons between the two: schools closing, stores closing, travel restrictions, runs on cleaning supplies and groceries. Many readers, not to mention friends and family, who initially scoffed are no longer scoffing. I get many texts and emails every day saying something along the lines of “can you believe they just cancelled…?”
I’m a numbers guy, so I’ve been working diligently to come up with a formula that expressed the path the number of cases and deaths was taking. The problem is that only a small number of cases have resolved in both Italy and the US.
Total cases in the US are (supposedly) 2,269. This is no doubt very far short of the actual number due to the lack of available testing. But, the outcome data are telling. Only 79 of these 2,269 are closed: 39% due to the patients’ recovery and 61% due to their death. This leaves 2,190 in limbo, whose fate is as yet undetermined. But, we can make some educated guesses.
While the cases are almost certainly undercounted, the number of deaths is probably fairly accurate. At 48 total deaths, the current mortality rate is 2.1%. Some might take solace in such a low number. But, that would probably be a mistake. The Italy data are below.
| Italy | ||
| date | cases | deaths |
| 21-Feb | 21 | 1 |
| 22-Feb | 79 | 2 |
| 23-Feb | 152 | 2 |
| 24-Feb | 229 | 6 |
| 25-Feb | 322 | 11 |
| 26-Feb | 400 | 12 |
| 27-Feb | 655 | 17 |
| 28-Feb | 889 | 21 |
| 29-Feb | 1,128 | 29 |
| 1-Mar | 1,701 | 34 |
| 2-Mar | 2,036 | 52 |
| 3-Mar | 2,502 | 79 |
| 4-Mar | 3,089 | 107 |
| 5-Mar | 3,858 | 148 |
| 6-Mar | 4,636 | 197 |
| 7-Mar | 5,883 | 233 |
| 8-Mar | 7,375 | 366 |
| 9-Mar | 9,172 | 463 |
| 10-Mar | 10,149 | 631 |
| 11-Mar | 12,462 | 827 |
| 12-Mar | 15,113 | 1,016 |
| 13-Mar | 17,660 | 1,266 |
| US | ||
| date | cases | deaths |
| 3-Mar | 124 | 9 |
| 4-Mar | 158 | 11 |
| 5-Mar | 221 | 12 |
| 6-Mar | 319 | 15 |
| 7-Mar | 435 | 19 |
| 8-Mar | 541 | 22 |
| 9-Mar | 704 | 26 |
| 10-Mar | 994 | 30 |
| 11-Mar | 1,301 | 38 |
| 12-Mar | 1,697 | 41 |
| 13-Mar | 2,269 | 48 |
| US – #1 | ||
| date | cases | deaths |
| 3-Mar | 124 | 9 |
| 4-Mar | 158 | 11 |
| 5-Mar | 221 | 12 |
| 6-Mar | 319 | 15 |
| 7-Mar | 435 | 19 |
| 8-Mar | 541 | 22 |
| 9-Mar | 704 | 26 |
| 10-Mar | 994 | 30 |
| 11-Mar | 1,301 | 38 |
| 12-Mar | 1,697 | 41 |
| 13-Mar | 2,269 | 48 |
| 14-Mar | 3,038 | 57 |
| 15-Mar | 4,066 | 67 |
| 16-Mar | 5,444 | 80 |
| 17-Mar | 7,288 | 94 |
| 18-Mar | 9,756 | 112 |
| 19-Mar | 13,061 | 132 |
| 20-Mar | 17,485 | 157 |
| 21-Mar | 23,407 | 185 |
| 22-Mar | 31,336 | 219 |
| 23-Mar | 41,950 | 260 |
| 24-Mar | 56,160 | 308 |
 At today’s press conference / pep rally, President Trump insisted on shaking hands with nearly every one of the corporate executives who got up to tout his company’s efforts – each of whom also reached out and adjusted the potentially infected microphone.
Trump then refused to admit he had shaken hands with or palled around with several individuals who were known to have tested positive, and was nonchalant about getting tested himself. Not a great example, to say the least. Do yourself a favor: Listen to the scientists and doctors and ignore the politicians.
I’ll continue to update the above numbers as conditions warrant. I hope I’m very, very wrong – but fear I’m not. Watch this space, and please be careful out there.
At today’s press conference / pep rally, President Trump insisted on shaking hands with nearly every one of the corporate executives who got up to tout his company’s efforts – each of whom also reached out and adjusted the potentially infected microphone.
Trump then refused to admit he had shaken hands with or palled around with several individuals who were known to have tested positive, and was nonchalant about getting tested himself. Not a great example, to say the least. Do yourself a favor: Listen to the scientists and doctors and ignore the politicians.
I’ll continue to update the above numbers as conditions warrant. I hope I’m very, very wrong – but fear I’m not. Watch this space, and please be careful out there.















Comments
One response to “COVID-19: What to Expect”
It is scary. One week makes a big difference. Just for thought. What will happen 3 months or 6 months from now?